
The word fibromyalgia comes from the Latin term for fibrous tissue (fibro) and the Greek ones for muscle (myo) and pain (algia). Fibromyalgia syndrome is chronic disorder which includes widespread muscle pain, fatigue, and multiple tender points that affects 3-6 million people in the United States. For reasons that are unclear, more than 90 percent of those who develop fibromyalgia are women. It is not currently known whether the predominance of women who suffer from fibromyalgia is a phenomenon of the socialization of women in the American culture or whether it is some combination of the female reproductive hormones and other genetic predispositions.
According to the American College of Rheumatology (ACR), fibromyalgia is defined as a history of pain in all four quadrants of the body lasting more than three months. Pain in all four quadrants means that you have pain in both your right and left sides, as well as above and below the waist. The ACR also described 18 characteristic tender points on the body that are associated with fibromyalgia. In order to be diagnosed with fibromyalgia, a person must have 11 or more tender points. In addition to pain and fatigue, people who have fibromyalgia may experience:
Fibromyalgia is often confused with another condition called "myofascial pain syndrome" or "myofascitis." Both fibromyalgia and myofascitis can cause pain in all four quadrants of the body and tend to have similar tender point locations, but the two conditions are worlds apart. Myofascitis is an inflammatory condition due to overuse or injury to your muscles, whereas fibromyalgia is caused by a stress-induced change in metabolism and healing. Myofascitis tend to come on rather suddenly and is usually associated with a particular activity or injury, true fibromyalgia has a slow, insidious onset, usually beginning in early adulthood. It is very important to diagnose each of these correctly, for they require very different approaches to treatment. Unfortunately, fibromyalgia is a chronic condition, meaning it lasts a long time - possibly a lifetime. However. it won't cause damage to your joints, muscles, or internal organs.
The latest research indicates that fibromyalgia is a stress-related condition that is a cousin in Systemic Lupus Erythematosis (often referred to as simply 'lupus') and Chronic Fatigue Syndrome. In all three of these conditions, there is the same predominantly female distribution, chronic fatigue, sleep disturbances, irritable bowel, as well as many other similarities. You can think about these three conditions as lying on a continuum with Fibromyalgia on one end, Lupus on the other and Chronic Fatigue Syndrome in the middle. All three of these conditions are caused by an abnormal stress response in the body, but with Lupus, the immune system is primarily affected, causing an autoimmune reaction that attacks your healthy tissues. On the other end of the spectrum is fibromyalgia, where metabolic abnormalities are primary. These metabolic changes are the result of a stress-induced decrease in blood flow to an area of the brain called the pituitary. This, in turn causes a decrease in a number of important hormones, such as the growth hormone releasing hormone (somatotropin) and the thyroid stimulating hormone. These hormonal changes lead to abnormal muscle healing, borderline or full-blown hypothyroid, as well as memory and cognitive changes.
One of the major physical abnormalities that occurs with fibromyalgia lies in the muscle itself, where there is a build up of a protein called "Ground Substance." Ground substance is normally found in muscle, bone and connective tissue all over the body and is responsible for making the tissues stronger and less susceptible to tearing. In a normal person, when a muscle is injured, the muscle tissue itself is able to regenerate and over time, completely heal itself. In a person with fibromyalgia, the muscle is unable to completely heal itself. Instead, an abnormally large amount of ground substance builds up in the injured area. It is the ground substance, coupled with local muscle spasm it creates that creates the muscle 'knots' associated with fibromyalgia.
A number of tests may be done to rule out other disorders and an examination can reveal whether a person has the characteristic tender areas on the back of the neck, shoulders, sternum, lower back, hips, shins, elbows, or knees. Unlike its cousin lupus, there are currently no diagnostic laboratory tests for fibromyalgia. Because there are no clinical tests for fibromyalgia, some doctors, unfortunately, conclude that a patient's pain is not real, or they may tell them that there is little they can do. But a combination of chiropractic, trigger point therapy, and lifestyle changes has proven to be very effective in decreasing the severity and duration of the physical pain and disability of fibromyalgia.
Fibromyalgia can be difficult to treat. Not all doctors are familiar with fibromyalgia and its treatment, so it is important to find a doctor who is. Fibromyalgia treatment often requires a team approach, utilizing chiropractic care, trigger point therapy, massage, dietary changes, as well as exercises and stretching.
Chiropractic care is critical for those who suffer from fibromyalgia in order to keep the spine and muscles from losing too much movement. Because fibromyalgia causes the muscles to tighten up and lose some of their natural pliability, it results in a global loss of movement in the spine. The loss of movement in the spine results in a neurological reflex that causes the muscles to tighten further. This vicious cycle will continue and over time will lead to increased pain, increased muscle tightness, a loss of movement, more difficulty sleeping and the development of more and more trigger points.
The only option is to continually adjust the spine and keep it moving. It is not uncommon for those with fibromyalgia to be adjusted three to four times per month to keep everything mobile and relaxed. The biggest concern in treating people with fibromyalgia is that their muscles have a diminished healing ability. For this reason, chiropractic adjustments are usually modified slightly to be more gentle than normal. This helps to decrease the stress on all of the small supporting muscles of the spine, which can be easily injured. It is important when seeking chiropractic care, to make sure that the doctor is familiar with the muscular changes that occur with fibromyalgia so that they can adjust their treatment accordingly.
The overwhelming characteristic of fibromyalgia is long-standing, body-wide pain with defined tender points, and frequently, trigger points. Trigger points are often confused with "tender points." They are not the same. A trigger point needs firm pressure to elicit pain, while tender points are painful with even very light pressure. Trigger points will refer pain to other areas of the body, whereas tender points will not. Unlike tender points, trigger points can occur in isolation and represent a source of radiating pain, even in the absence of direct pressure. As discussed earlier, trigger points are purely comprised of spasmed muscle fibers, whereas tender points are knots filled with ground substance. Those with fibromyalgia almost always have a combination of the two - trigger points and tender points - and can improve dramatically with light trigger point therapy.
Trigger point therapy for fibromyalgia is much like trigger point therapy for low back pain, neck pain or headaches. The points are the same. The difference is just intensity. Since the muscles in patients with fibromyalgia are easily injured and take longer to heal, it is necessary to use less pressure on their trigger points.
Since poor healing of muscle tissue and chronic pain are characteristic traits of fibromyalgia, laser therapy is an important part of any treatment plan. Two of the major benefits of cold laser therapy is stimulation of tissue healing and decreased sensations of pain.
A 1997 study of 846 people with fibromyalgia reported in the Journal of Clinical Laser Medicine and Surgery demonstrated that two-thirds of the patients experienced improved pain and mobility with cold laser therapy. Another study published in Rheumatology International in 2002, showed that those who received laser therapy had a significant improvement in pain, fatigue and morning stiffness.
Your day to day lifestyle choices have a tremendous impact on how much impact fibromyalgia will have on your life. The difference between those who take care of themselves and those who do not is tremendous. Those who make lifestyle changes to help their fibromyalgia suffer much less pain, are able to remain more active and have a much higher quality of life than those who do not. If you have fibromyalgia, here are some of the main things that you can do on a daily basis to help your body:
-Getting enough sleep and the right kind of sleep can help ease the pain and fatigue of fibromyalgia, but is something that can be hard to get. Many people with fibromyalgia have problems such as pain, restless legs syndrome and brain-wave irregularities that interfere with restful sleep. Insomnia is very common. Although alcohol may help you to relax, it is not recommended before bed as it has been shown to interfere with restful sleep. Some of those with fibromyalgia have found 5-hydroxy tryptophan (5-HTP) very helpful, as well as the prescription anti-depressant amitriptyline. Typically, we don't recommend taking perscritpion drugs, but in this case, it is difficult to heal without enough sleep.
- Improved fitness through exercise is recommended. Studies have shown that fibromyalgia symptoms can be relieved by aerobic exercise. Though pain and fatigue may make exercise and daily activities difficult, it's crucial to be as physically active as possible. The best way to begin a fitness program is to start with low impact exercises, like walking and swimming. Starting slowly helps stretch and mobilize tight, sore muscles. High-impact aerobics and weight lifting could cause increased discomfort, so pay attention to your body. The more you can exercise, the better off you will be.
-Most people with fibromyalgia are able to continue working, but they may have to make big changes to do so. It may be necessary to reduce the number of hours at work, find a job that will allow you to have a flexible schedule, or switch to a less physically demanding job. Many people with fibromyalgia require specially designed office chairs, adjustable desks or other adaptations in order to continue working. If you face obstacles at work, such as an uncomfortable desk chair that leaves your back aching or difficulty lifting heavy boxes or files, your employer may make adaptations that will enable you to keep your job.
-Foods, just like anything else, have the ability to either stress your body or to help your body heal. Foods that tend to be stressful on the body include: dairy, eggs, wheat, corn, as well as anything with monosodium glutamate (MSG), nitrates or nitrites (as are found in processed foods). Several environmental toxins may also contribute to the overall physical stress on your body, therefore fish should be avoided as well. It is important that you eat as much clean, organically grown fresh foods as possible. Base your diet around whole foods such as: brown rice, legumes, oats, spelt, rice milk, soy, hormone-free chicken or turkey, roots, nuts and berries.
-There are dozens of nutritional products that claim to be 'the answer' for fibromyalgia. To date, none of them have proven to be of much long-term benefit for anyone. However, there are some people who have used magnesium malate with good results, some people who have used ginkgo biloba with good results and others with various herbals. The bottom line with nutritional supplements is that, to date, there is nothing that works for everyone. If you come across something that you would like to try, by all means do so, as long as you check it out with your chiropractor first to ensure that it won't interfere with any of your other treatment. Contact us today!

Shin splints are characterized by pain in the front part of the lower leg. It occurs on the inside edge of the large bone there — the tibia. This condition is common in runners, but can also occur in other physically active people.
Shin splints usually happen during or after a change in the intensity of physical activity, such as running more miles or more frequently.
Shin splints are not a standard medical diagnosis. The condition may also be called medial tibial stress syndrome (MTSS), anterior tibial pain or exercise-induced leg pain.
Shin splints are very common among professional and recreational athletes, especially runners, military recruits and dancers.
Overuse of the leg muscles — without taking enough time to rest and heal — can lead to inflammation or swelling of the tendons, muscles or tissue covering the shin.
This causes pain along the front of the shin. Symptoms range from a dull, tight feeling to a sharp pain along the shin.
Several factors increase your chance of developing shin splints, such as:
In addition to excessive training, other conditions can also lead to pain in the shins, such as:
Shin splints will often go away with basic therapy, which involves:
However, if the shin splits don't clear up quickly, your chiropractor will look for other problems that may be contributing to the pain. This includes examining your spine, hips, knees and feet for misalignments.
One problem with the foot that can lead to shin splints is over pronation — or “rolling in” of the foot. This condition causes overstretching in the shin muscles. If this is the case, your chiropractor may prescribe a foot orthotic for you. This will adjust how your foot strikes the ground.
Your chiropractor may also make adjustments in your foot joints, ankle, knee, SI joint or low back. This can relieve the pain from shin splints, or prevent them from happening again.
If you have shin splints, look for a chiropractor who specializes in treating sports injuries and conditions. This will help you return to your regular training program.
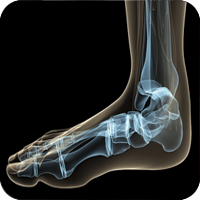
About 90 percent of people will recover from plantar fasciitis within a few months following conservative treatment.
Plantar fasciitis is one of the most common explanations of heel pain. It is caused by inflammation to the thick band that connects the toes to the heel bone, called the plantar fascia, which runs across the bottom of your foot. The condition is most commonly seen in runners, pregnant women, overweight people, and individuals who wear inadequately supporting shoes. Plantar fasciitis typically affects people between the ages of 40 and 70.
Plantar fasciitis commonly causes a stabbing pain in the heel of the foot, which is worse during the first few steps of the day after awakening. As you continue to walk on the affected foot, the pain gradually lessens. Usually, only one foot is affected, but it can occur in both feet simultaneously.
To diagnose plantar fasciitis, your doctor will physically examine your foot by testing your reflexes, balance, coordination, muscle strength, and muscle tone. Your doctor may also advise a magnetic resonance imaging (MRI) or X-ray to rule out other others sources of your pain, such as a pinched nerve, stress fracture, or bone spur.
Treatment for plantar fasciitis includes chiropractic care, medication, physical therapy, shock wave therapy, or surgery.
Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen are used to treat the inflammation and pain of plantar fasciitis, but they won't cure the condition. Corticosteroids can also be used to ease pain and reduce inflammation. Corticosteroids are applied either as a topical solution in conjunction with a non-painful electric current or through injections to the affected area.
Stretching exercises for the Achilles tendon and plantar fascia are recommend to relieve pain and aid in the healing process. Sometimes application of athletic tape is recommended. In moderate or severe cases of plantar fasciitis, your doctor may recommend you wearing a night splint, which will stretch the arch of your foot and calf while you sleep. This helps to lengthen the Achilles tendon and plantar fascia for symptom relief. Depending on the severity of your plantar fasciitis, your physician may prescribe a store-bought orthotic (arch support) or custom-fitted orthotic to help distribute your foot pressure more evenly.
When more conservative methods have failed to reduce plantar fasciitis pain, your doctor may suggest extracorporeal shock wave therapy, which is used to treat chronic plantar fasciitis. Extracorporeal shock wave therapy uses sound waves to stimulate healing, but may cause bruises, numbness, tingling, swelling, and pain. When all else fails, surgery may be recommended to detach the plantar fascia from the heel bone. Few people need surgery to treat the condition.
Stretching your plantar fasciitis is something you can do at home to relieve pain and speed healing. Ice massage performed three to four times per day in 15 to 20 minute intervals is also something you can do to reduce inflammation and pain. Placing arch supports in your shoes absorbs shock and takes pressure off the plantar fascia.
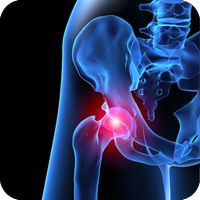
Patients will find that chiropractic care for hip and knee osteoarthritis can help reduce inflammation, improve joint functioning, reduce pain, and strengthen the muscles around the affected joints.
Osteoarthritis in the knee and hip areas can be a very painful injury, and one that is often a chronic condition if left untreated. Chiropractic care for hip osteoarthritis and knee osteoarthritis can be very helpful for patients who have been unable to find relief from the pain in any other way.
Signs of hip osteoarthritis and knee osteoarthritis include an increasing level of pain in the hip area that may extend into the groin area, pain shooting down the thighs, and pain in the knee joints. It is not uncommon for the knees to be the first place the pain is felt, and some patients may not notice the hip pain until later. The pain often increases when the weather is colder, or when the patient is engaged in physical activity like jogging or walking.
Chiropractors use very gentle spinal adjustments to place the spinal column in proper alignment, which has a positive effect on the hip joints that are connected to the spine. While hip and knee osteoarthritis is not curable at this time, it is very much manageable with the help of chiropractic care.
Knee osteoarthritis can also be managed very effectively with the help of chiropractic care. The treatments for both knee and hip osteoarthritis may be similar, and can include stretching, massage, gentle manipulation of any painful joints, and the use of ultrasound for healing.
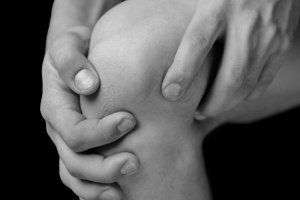
Knee pain is common in people of all ages. It may start suddenly — such as after exercise or an injury. But it can also develop over time, starting out as minor discomfort.
Chiropractic care for knee pain includes first identifying the underlying cause of the pain, which could be an injury, mechanical problem or some kind of arthritis. Once this is known, the chiropractor can determine the best treatment for the pain.
There are three main types of problems that can lead to pain in the knee.
Damaging any part of the knee may cause pain. These parts include:
Some of the most common knee injuries include:
Changes in how the knee works can lead to pain in the knee, such as:
There are many different types of arthritis that can cause swelling and pain in the knee, including:
Chiropractors will first do a thorough physical examination. This will enable them to identity the underlying cause of the knee pain. Even though the pain is located in the knee, the problem can lie elsewhere in the body.
For example, runners often complain of a tight iliotibial (IT) band — a common condition for them. This, however, may be caused by weakness in certain muscles, which makes them walk or run unevenly. In order to stabilize the joints, the IT band has to work harder. Over time, this may cause it to tighten and lead to knee pain.
Chiropractic care may be able to relieve knee pain, especially when combined with standard medical care. Spine and joint manipulation can improve the functioning of the knee by:
Chiropractors may also use other techniques to reduce inflammation in the knee that is causing pain, such as ultrasound therapy or ice massage. They may also apply special kinds of tape to the body to treat ligament injuries. This helps stabilize the problem area and reduce inflammation.
Excessive knee pain can often lead to people avoiding certain activities, such as walking, running or biking. Over time, the lack of physical activity can lead to other health problems and may aggravate the pain in the knee.
Early treatment of knee pain, along with the underlying causes, can help people return to their normal activities sooner. This will improve their health both in the short and long term. It will also allow athletes to return to their training and competitions.
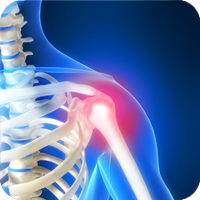
Chiropractors will always seek to treat shoulder pain with the most gentle and drug-free methods possible. The ultimate goal of chiropractic care for shoulder pain is to bring the patient's shoulder back to full function while reducing and eliminating the pain caused by the injury.
Shoulder pain can have a number of different causes, ranging from an injury like a car accident, to a chronic problem like arthritis. Patients who experience shoulder pain may be surprised by the intensity and duration of the pain. The shoulder area is so essential for completing daily activities that it makes sense that the shoulder pain injury should be taken seriously and treated to avoid worsening your condition.
Some signs that shoulder pain needs immediate attention may include a decreased ability to hold objects, decreased functioning of the arm, shoulder pain that persists even while at rest, shoulder pain that lasts more than a day or two, and unusual twinges or aches in the shoulder area.
Chiropractic care can be an extremely effective treatment for shoulder pain regardless of its cause. A chiropractor will often begin with an examination of the patient's neck area since shoulder pain can frequently be the result of "referred" pain from the neck. Whether the shoulder pain is connected to the neck or is limited to the lower part of the shoulder, it can generally be treated with non-invasive methods of natural healing such as chiropractic care.
Care for an injured shoulder may include application of heat, application of ice packs, gentle manipulation from the chiropractor to help the shoulder return to its original state of functionality, and gentle stretching and strengthening exercises that the patient can perform at home.

Most neck and upper back pain is caused by a combination of factors, including injury, poor posture, chiropractic subluxations, stress, and in some instances, disc problems.
Most people do not realize how much they move their neck during the day until they are unable to do so. The degree of flexibility of the neck, coupled with the fact that it has the least amount of muscular stabilization and it has to support and move your 14 - 16 pound head, means that the neck is very susceptible to injury. You can picture your neck and head much like a bowling ball being held on top of a stick by small, thin, elastic bands. It doesn't take much force to disrupt that delicate balance.
The spinal cord runs through a space in the vertebrae to send nerve impulses to every part of the body. Between each pair of cervical vertebrae, the spinal cord sends off large bundles of nerves that run down the arms and to some degree, the upper back. This means that if your arm is hurting, it may actually be a problem in the neck! Symptoms in the arms can include numbness, tingling, cold, aching, and "pins and needles".
These symptoms can be confused with carpal tunnel syndrome, a painful condition in the hands that is often found in people who work at computer keyboards or perform other repetitive motion tasks for extended periods. Problems in the neck can also contribute to headaches, muscle spasms in the shoulders and upper back, ringing in the ears, otitis media (inflammation in the middle ear, often mistaken for an ear infection in children), temporomandibular joint dysfunction (TMJ), restricted range of motion and chronic tightness in the neck and upper back.
We associate the neck and upper back together, because most of the muscles that are associated with the neck either attach to, or are located in, the upper back. These muscles include the trapezius, the levator scapulae, the cervical paraspinal muscles and the scalenes, as well as others.
Most neck and upper back pain is caused by a combination of factors, including injury, poor posture, chiropractic subluxations, stress, and in some instances, disc problems.
By far, the most common injury to the neck is a whiplash injury. Whiplash is caused by a sudden movement of the head, either backward, forward, or sideways, that results in the damage to the supporting muscles, ligaments and other connective tissues in the neck and upper back. Whether from a car accident, sports, or an accident at work, whiplash injuries need to be taken very seriously. Because symptoms of a whiplash injury can take weeks or months to manifest, it is easy to be fooled into thinking that you are not as injured as you really are. Too often people don't seek treatment following a car accident or sports injury because they don't feel hurt. Unfortunately, by the time more serious complications develop, some of the damage from the injury may have become permanent. Numerous studies have shown that years after whiplash victims settle their insurance claims, roughly half of them state that they still suffer with symptoms from their injuries. If you have been in a motor vehicle or any other kind of accident, don't assume that you escaped injury if you are not currently in pain. Get checked out by a good chiropractor.
Forward head posture is very common for people who are stooped over their computers all day long. If not taken care of with chiropractic care, subluxations like this can worsen over time.
One of the most common causes of neck pain, and sometimes headaches, is poor posture. It's easy to get into bad posture habits without even realizing it - even an activity as "innocent" as reading in bed can ultimately lead to pain, headaches, and more serious problems. The basic rule is simple: keep your neck in a "neutral" position whenever possible. Don't bend or hunch your neck forward for long periods. Also, try not to sit in one position for a long time. If you must sit for an extended period, make sure your posture is good: Keep your head in a neutral position, make sure your back is supported, keep your knees slightly lower than your hips, and rest your arms if possible.
Subluxations in the neck and upper back area are extremely common due to the high degree of stress associated with holding up your head, coupled with the high degree of instability in the cervical spine. Most subluxations tend to be centered around four areas: the top of the cervical spine where it meets the skull; in the middle of the cervical spine where the mechanical stress from the head is the greatest; in the transition where the cervical and thoracic areas of the spine meet; and in the middle of the thoracic spine where the mechanical stress from the weight of the upper body is greatest. Signs of subluxation include looking in the mirror and seeing your head tilted or one shoulder higher than the other. Often women will notice that their sleeve length is different or that a necklace is hanging off center. If someone looks at you from the side they may notice that your head sits forward from your shoulders. This is known as FHP - forward head posture - and is very common for people who are stooped over their computers all day long. Subluxations are a debt to the body. If they are not taken care of soon after they occur, then they can get much worse over time due to the accumulation of compounding interest.
When most people become stressed, they unconsciously contract their muscles. In particular, the muscles in their back. This 'muscle guarding' is a survival response designed to guard against injury. In today's world where we are not exposed to physical danger most of the time, muscle guarding still occurs whenever we become emotionally stressed. The areas most affected are the muscles of the neck, upper back and low back. For most of us, the particular muscle affected by stress is the trapezius muscle, where daily stress usually leads to chronic tightness and the development of trigger points.
The two most effective ways you can reduce the physical effects of stress on your own are to increase your activity level - exercise - and by deep breathing exercises. When you decrease the physical effects of stress, you can substantially reduce the amount of tightness and pain in your upper back and neck.
The discs in your cervical spine can herniate or bulge and put pressure on the nerves that exit from the spine through that area. Although cervical discs do not herniate nearly as often as lumbar discs do, they occasionally can herniate, especially when the discs sustain damage from a whiplash injury. Contact us today!

The term "whiplash" was first used in 1928 to define an injury mechanism of sudden hyperextension followed by an immediate hyperflexion of the neck that results in damage to the muscles, ligaments and tendons - especially those that support the head. Today, we know that whiplash injuries frequently do not result from hyperextension or hyperflexion (extension and flexion beyond normal physiological limits), but rather an extremely rapid extension and flexion that causes injuries.
Due to their complicated nature and profound impact on peoples lives, few topics in health care generate as much controversy as whiplash injuries. Unlike a broken bone where a simple x-ray can validate the presence of the fracture and standards of care can direct a health care professional as to the best way in which to handle the injury, whiplash injuries involve an unpredictable combination of nervous system, muscles joints and connective tissue disruption that is not simple to diagnose and can be even more of a challenge to treat. In order to help you understand the nature of whiplash injuries and how they should be treated, it is necessary to spend a bit of time discussing the mechanics of how whiplash injuries occur.
During a rear-end automobile collision, your body goes through an extremely rapid and intense acceleration and deceleration. In fact, all four phases of a whiplash injury occur in less than one-half of a second! At each phase, there is a different force acting on the body that contributes to the overall injury, and with such a sudden and forceful movement, damage to the vertebrae, nerves, discs, muscles, and ligaments of your neck and spine can be substantial.
During this first phase, your car begins to be pushed out from under you, causing your mid-back to be flattened against the back of your seat. This results in an upward force in your cervical spine, compressing your discs and joints. As your seat back begins to accelerate your torso forward, your head moves backward, creating a shearing force in your neck. If your head restraint is properly adjusted, the distance your head travels backward is limited. However, most of the damage to the spine will occur before your head reaches your head restraint. Studies have shown that head restraints only reduce the risk of injury by 11-20 percent.
During phase two, your torso has reached peak acceleration - 1.5 to 2 times that of your vehicle itself - but your head has not yet begun to accelerate forward and continues to move rearward. An abnormal S-curve develops in your cervical spine as your seat back recoils forward, much like a springboard, adding to the forward acceleration of the torso. Unfortunately, this forward seat back recoil occurs while your head is still moving backward, resulting in a shearing force in the neck that is one of the more damaging aspects of a whiplash injury. Many of the bone, joint, nerve, disc and TMJ injuries that I see clinically occur during this phase.
During the third phase, your torso is now descending back down in your seat and your head and neck are at their peak forward acceleration. At the same time, your car is slowing down. If you released the pressure on your brake pedal during the first phases of the collision, it will likely be reapplied during this phase. Reapplication of the brake causes your car to slow down even quicker and increases the severity of the flexion injury of your neck. As you move forward in your seat, any slack in your seat belt and shoulder harness is taken up.
This is probably the most damaging phase of the whiplash phenomenon. In this fourth phase, your torso is stopped by your seat belt and shoulder restraint and your head is free to move forward unimpeded. This results in a violent forward-bending motion of your neck, straining the muscles and ligaments, tearing fibers in the spinal discs, and forcing vertebrae out of their normal position. Your spinal cord and nerve roots get stretched and irritated, and your brain can strike the inside of your skull causing a mild to moderate brain injury. If you are not properly restrained by your seat harness, you may suffer a concussion, or more severe brain injury, from striking the steering wheel or windshield.
As we discussed briefly in the introduction, whiplash injuries can manifest in a wide variety of ways, including neck pain, headaches, fatigue, upper back and shoulder pain, cognitive changes and low back pain. Due to the fact that numerous factors play into the overall whiplash trauma, such as direction of impact, speed of the vehicles involved, as well as gender, age and physical condition, it is impossible to predict the pattern of symptoms that each individual will suffer. Additionally, whiplash symptoms commonly have a delayed onset, often taking weeks or months to present. There are, however, a number of conditions that are very common among those who have suffered from whiplash trauma.
It is the single most common complaint in whiplash trauma, being reported by over 90 percent of patients. Often this pain radiates across the shoulders, up into the head, and down between the shoulder blades. Whiplash injuries tend to affect all of the tissues in the neck, including the facet joints and discs between the vertebrae, as well as all of the muscles, ligaments and nerves.
Facet joint pain is the most common cause of neck pain following a car accident. Facet joint pain is usually felt on the back of the neck, just to the right or left of center, and is usually tender to the touch. Facet joint pain cannot be visualized on x-rays or MRIs. It can only be diagnosed by physical palpation of the area.
Disc injury is also a common cause of neck pain; especially chronic pain. The outer wall of the disc (called the anulus) is made up of bundles of fibers that can be torn during a whiplash trauma. These tears, then, can lead to disc degeneration or herniation, resulting in irritation or compression of the nerves running through the area. This compression or irritation commonly leads to radiating pain into the arms, shoulders and upper back, and may result in muscle weakness.
Damage to the muscles and ligaments in the neck and upper back are the major cause of the pain experienced in the first few weeks following a whiplash injury, and is the main reason why you experience stiffness and restricted range of motion. But as the muscles have a chance to heal, they typically don't cause as much actual pain as they contribute to abnormal movement. Damage to the ligaments often results in abnormal movement and instability.
After neck pain, headaches are the most prevalent complaint among those suffering from whiplash injury, affecting more than 80 percent of all people. While some headaches are actually the result of direct brain injury, most are related to injury of the muscles, ligaments and facet joints of the cervical spine, which refer pain to the head. Because of this, it is important to treat the supporting structures of your neck in order to help alleviate your headaches.
A less common, but very debilitating disorder that results from whiplash is temporomandibular joint dysfunction (TMJ). TMJ usually begins as pain, clicking and popping noises in the jaw during movement. If not properly evaluated and treated, TMJ problems can continue to worsen and lead to headaches, facial pain, ear pain and difficulty eating. Many chiropractors are specially trained to treat TMJ problems, or can refer you to a TMJ specialist.
Believe it or not, mild to moderate brain injury is common following a whiplash injury, due to the forces on the brain during the four phases mentioned earlier. The human brain is a very soft structure, suspended in a watery fluid called cerebrospinal fluid. When the brain is forced forward and backward in the skull, the brain bounces off the inside of the skull, leading to bruising or bleeding in the brain itself. In some cases, patients temporarily lose consciousness and have symptoms of a mild concussion. More often, there is no loss of consciousness, but patients complain of mild confusion or disorientation just after the crash. The long-term consequences of a mild brain injury can include mild confusion, difficulty concentrating, sleep disturbances, irritability, forgetfulness, loss of sex drive, depression and emotional instability. Although less common, the nerves responsible for your sense of smell, taste and even your vision may be affected as well, resulting in a muted sense of taste, changes in your sensation of smell and visual disturbances.
Dizziness following a whiplash injury usually results from injury to the facet joints of the cervical spine, although in some cases injury to the brain or brain stem may be a factor as well. Typically, this dizziness is very temporary improves significantly with chiropractic treatment.
Although most people consider whiplash to be an injury of the neck, the low back is also commonly injured as well. In fact, low back pain is found in more than half of rear impact-collisions in which injury was reported, and almost three-quarters of all side-impact crashes. This is mostly due to the fact that the low back still experiences a tremendous compression during the first two phases of a whiplash injury, even though it does not have the degree of flexion-extension injury experienced in the neck.
With proper care, many mild whiplash injuries heal within six to nine months. However, more than 20 percent of those who suffer from whiplash injuries continue to suffer from pain, weakness or restricted movement two years after their accident. Unfortunately, the vast majority of these people will continue to suffer from some level of disability or pain for many years after that, if not for the rest of their lives.
Whiplash is a unique condition that requires the expertise of a skilled health professional specially trained to work with these types of injuries. The most effective treatment for whiplash injuries is a combination of chiropractic care, rehabilitation of the soft tissues and taking care of yourself at home.
Chiropractic care utilizes manual manipulation of the spine to restore the normal movement and position of the spinal vertebrae. It is by far the single-most effective treatment for minimizing the long-term impact of whiplash injuries, especially when coupled with massage therapy, trigger point therapy, exercise rehabilitation and other soft tissue rehabilitation modalities.
The term 'soft tissue' simply refers to anything that is not bone, such as your muscles, ligaments, tendons, nervous system, spinal discs and internal organs. During a whiplash injury, the tissues that are affected most are the soft tissues, the muscles, ligaments and discs in particular. In order to minimize permanent impairment and disability, it is important to use therapies that stimulate the soft tissues to heal correctly. These include massage therapy, electro-stimulation, trigger point therapy, stretching and specific strength and range of motion exercises.
The most effective chiropractic care and soft tissue rehabilitation will be limited in its benefit if what you do at home or at work stresses or re-injures you on a daily basis. For this reason, it is important that your plan of care extend into the hours and days between your clinic visits to help speed your recovery. Some of the more common home care therapies are the application of ice packs, limitations on work or daily activities, specific stretches and exercises, taking nutritional supplements and getting plenty of rest.
In some severe cases of whiplash, it may be necessary to have some medical care as part of your overall treatment plan. The most common medical treatments include the use of anti-inflammatory medications, muscle relaxants, trigger point injections and, in some cases, epidural spinal injections. These therapies should be used for short-term relief of pain, if necessary, and not be the focus of treatment. After all, a drug cannot restore normal joint movement and stimulate healthy muscle repair. Fortunately, surgery is only needed in some cases of herniated discs, when the disc is pressing on the spinal cord, and in some cases of spine fractures.

Eighty percent of people suffer from back pain at some point in their lives. Back pain is the second most common reason for visits to the doctor's office, outnumbered only by upper-respiratory infections. In fact, it is estimated that low back pain affects more than half of the adult population each year and more than 10 percent of all people experience frequent bouts of low back pain.
The susceptibility of the low back to injury and pain is due to the fact that the low back, like the neck, is a very unstable part of the spine. Unlike the thoracic spine, which is supported and stabilized by the rib cage. This instability allows us to have a great deal of mobility to touch our toes, tie our shoes or pick something up from the ground, but at the cost of increased risk of injury.
As long as it is healthy and functioning correctly, the low back can withstand tremendous forces without injury. Professional powerlifters can pick up several hundred pounds off the floor without injuring their low back. However, if the low back is out of adjustment or has weakened supporting muscles, something as simple as taking a bag of groceries out of the trunk of their car, picking something up off the floor, or even simply bending down to pet the cat can cause a low back injury.
Until recently, researchers believed that back pain would heal on its own. We have learned, however, that this is not true. Recent studies showed that when back pain is not treated, it may go away temporarily, but will most likely return. It is important to take low back pain seriously and seek professional chiropractic care. This is especially true with pain that recurs over and over again. Contact our chiropractor . . . we can help!
There are many different conditions that can result in low back pain, including: sprained ligaments, strained muscles, ruptured disks, trigger points and inflamed joints. While sports injuries or accidents can lead to injury and pain, sometimes even the simplest movements, like picking up a pencil from the floor, can have painful results. In addition, conditions such as arthritis, poor posture, obesity, psychological stress and even kidney stones, kidney infections, blood clots, or bone loss can lead to pain.
Due to the fact that there are a whole lot of things that can cause low back pain, and some of those things can be quite serious if left untreated, it is important to seek professional help. Chiropractors are the experts at diagnosing the cause and determining the proper treatment for low back pain. Here are some of the most common causes I see:
Whenever there is a disruption in the normal movement or position of the vertebrae, the result is pain and inflammation. In the lumbar spine, these usually occur at the transition between the lower spine and the sacrum. Subluxations can lead to debilitating low back pain. Fortunately, subluxations are easily treatable and often times a significant reduction in pain is experienced almost immediately after treatment.
Contrary to popular belief, a herniated disc does not automatically mean that you are going to suffer from low back pain. In fact, one study found that almost half of all adults had at least one bulging or herniated disc, even though they did not suffer any back pain from it. On the other hand, herniated discs can be a source of intense and debilitating pain that frequently radiates to other areas of the body. Unfortunately, once a disc herniates, they rarely, if ever, completely heal. Further deterioration can often be avoided through regular chiropractic care, but a complete recovery is much less common.
This is commonly the source of low back pain among the weekend warriors. You know, the type who have very little physical activity during the week, but once the weekend arrives, they push themselves way too much. By the end of the weekend, they are lying flat on their back counting down the hours before they can get in to see their chiropractor. Overworking the muscles or ligaments of the low back can lead to small tears in the tissues, which then become painful, swollen, and tight.
Whenever you become stressed, your body responds by increasing your blood pressure and heart rate, flooding your body with stress hormones and tightening up your muscles. When you are stressed all the time, the chronic tension causes your muscles to become sore, weak and loaded with trigger points. If you are stressed out all of the time and you have low back pain, it is important to do some relaxation exercises, such as deep breathing, as well as to get regular exercise.
Chiropractic treatment for low back pain is usually pretty straightforward. Most commonly, it's simply a matter of adjusting the lower lumbar vertebrae and pelvis to re-establish normal motion and position of your bones and joints.
Chiropractic for the low back has been repeatedly shown to be the most effective treatment for low back pain. In fact, major studies have shown that chiropractic care is more effective, cheaper and has better long-term outcomes than any other treatment. This makes sense because chiropractic care is the only method of treatment that serves to re-establish normal vertebral motion and position in the spine. All other treatments, such as muscle relaxants, pain killers, and bed rest, only serve to decrease the symptoms of the problem and do not correct the problem itself.

Headaches affect just about everyone at some point and they can present themselves in many different ways. Some people only experience pain in one part of their head or behind their eyes, some people experience a pounding sensation inside their whole head, and some people even experience nausea, while others do not. The pain itself may be dull or sharp and may last for anywhere from a few minutes to a few days. Fortunately, very few headaches have serious underlying causes, but those that do require urgent medical attention.
Although headaches can be due to a wide variety of causes, such as drug reactions, temporomandibular joint dysfunction (TMJ), tightness in the neck muscles, low blood sugar, high blood pressure, stress and fatigue, the majority of recurrent headaches are of two types: tension headaches (also called cervicogenic headaches) and migraine headaches. There is a third, less common, type of headaches called a cluster headache that is a cousin to the migraine.
Numerous research studies have shown that chiropractic adjustments are very effective for treating tension headaches, especially headaches that originate in the neck.
A report released in 2001 by researchers at the Duke University Evidence-Based Practice Center in Durham, NC, found that "spinal manipulation resulted in almost immediate improvement for those headaches that originate in the neck, and had significantly fewer side effects and longer-lasting relief of tension-type headache than commonly prescribed medications." These findings support an earlier study published in the Journal of Manipulative and Physiological Therapeutics that found spinal manipulative therapy to be very effective for treating tension headaches. This study also found that those who stopped chiropractic treatment after four weeks continued to experience a sustained benefit in contrast to those patients who received pain medication.
Each individual's case is different and requires a thorough evaluation before a proper course of chiropractic care can be determined. However, in most cases of tension headaches, significant improvement is accomplished through manipulation of the upper two cervical vertebrae, coupled with adjustments to the junction between the cervical and thoracic spine. This is also helpful in most cases of migraine headaches, as long as food and lifestyle triggers are avoided as well.
Trigger point therapy for headaches tends to involve four muscles: the Splenius muscles, the Suboccipitals, the Sternocleidomastoid (SCM) and the Trapezius. The Splenius muscles are comprised of two individual muscles - the Splenius Capitis and the Splenius Cervicis. Both of these muscles run from the upper back to either the base of the skull (splenius capitis) or the upper cervical vertebrae (splenius cervicis). Trigger points in the Splenius muscles are a common cause of headache pain that travels through the head to the back of the eye, as well as to the top of the head.
The Suboccipitals are actually a group of four small muscles that are responsible for maintaining the proper movement and positioning between the first cervical vertebra and the base of the skull. Trigger points in these muscles will cause pain that feels like it's inside the head, extending from the back of the head to the eye and forehead. Often times it will feel like the whole side of the head hurts, a pain pattern similar to that experienced with a migraine.
The Sternocleidomastoid (SCM) muscle runs from the base of the skull, just behind the ear, down the side of the neck to attach to the top of the sternum (breastbone). Although most people are not aware of the SCM trigger points, their effects are widespread, including referred pain, balance problems and visual disturbances. Referred pain patterns tend to be deep eye pain, headaches over the eye and can even cause earaches. Another unusual characteristic of SCM trigger points is that they can cause dizziness, nausea and unbalance.
The trapezius muscle is the very large, flat muscle in the upper and mid back. A common trigger point located in the very top of the Trapezius muscle refers pain to the temple and back of the head and is sometimes responsible for headache pain. This trigger point is capable of producing satellite trigger points in the muscles in the temple or jaw, which can lead to jaw or tooth pain.
Contact us today!
